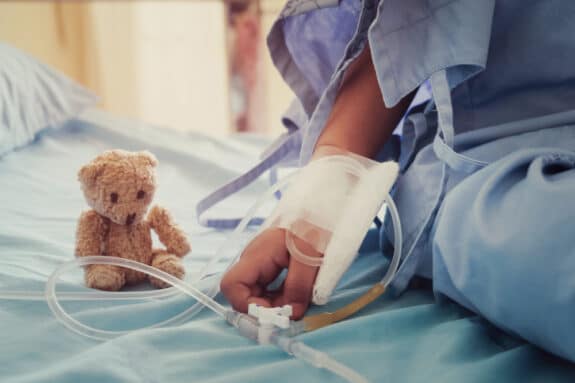
Acute lymphoblastic leukemia, or ALL, affects some 3,000 children and adults each year. Most of them do survive, but around 15 percent ultimately relapse, despite treatment and technology. Now there is a new treatment on the horizon – a gene therapy in which a person’s own blood cells are turned into a cancer-fighting army. One of just many “living drugs” under development, this therapy has just gained approval from the Food and Drug Administration.
“This is a brand new way of treating cancer,” said Dr. Stephan Grupp of Children’s Hospital of Philadelphia, who treated the first child with CAR-T cell therapy — a girl who had been near death at the time, but is cancer-free, five years later. “That’s enormously exciting.”
Made from scratch for every patient, the CAR-T treatment does not stop the disease. Instead, it turbo-charges the body’s own T-cells, immune system soldiers that fight infections and illnesses in the body. They are reprogrammed to harbor a “chimeric antigen receptor,” or CAR, that hones in on the cancer cells and attacks them – something T-cells often struggle to do since cancer cells often fly under the radar, undetected.
“We’re entering a new frontier in medical innovation with the ability to reprogram a patient’s own cells to attack a deadly cancer,” said FDA Commissioner Scott Gottlieb.
Developed by Novartis and the University of Pennsylvania, the therapy has been approved for use in several hundred patients per year. Most are in devastating situations, extremely ill from leukemia. If the key study is any indication, as many as 80 percent may go into remission soon after receiving the treatment. However, there are a few concerns and warnings.
First, leukemia is an aggressive cancer, so it could overtake the patient before the genetically altered T-cells can be returned to their body. Second, leukemia may develop a resistance to the T-cells. Lastly, there are some highly concerning side effects, including an immune system overreaction called “cytokine release syndrome,” which can result in high fever, plummeting blood pressure, and potential organ damage.
“This is remarkable technology,” said Dr. Mikkael Sekeres of the American Society of Hematology. He cautioned, however, that CAR-T “isn’t a panacea.”
Because of those risks, patients must go to a specially trained and certified treatment center to receive gene therapy. A total of 32 are expected to go up across the country, the first 20 of which are expected to start treatment within the next month. The cost for the therapy comes in at almost half a million dollars – about the price of a bone marrow transplant – but it may be the only treatment that is needed. In fact, researchers say that the T-cells may continue fighting against remission for years.
“I don’t want to be an apologist for high drug prices in the U.S.,” Grupp stressed. But if it’s the last treatment they need, “that’s a really significant one-time investment in their wellness, especially in kids who have a whole lifetime ahead of them.”