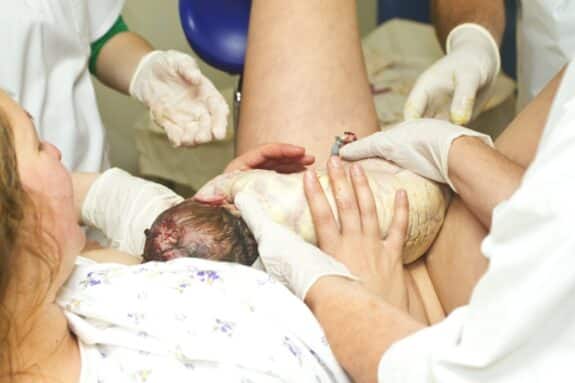
Canadian athlete, Aly Jenkins, recently died from a complication during childbirth known as an amniotic embolism. Though rare, this condition is both difficult to detect and extremely deadly. Its prevalence is also increasing throughout much of the world, which is why medical professionals want to raise more awareness about the condition.
So what, exactly, is an amniotic embolism and how does one occur – and even more importantly, is there a way to prevent, cure, or detect it?
Amniotic Embolisms
An amniotic embolism occurs when amniotic fluid or fetal material enters the mother’s bloodstream. Health experts believe the most common cause is a breakdown in the placental barrier, which could be caused by trauma or a variety of other factors.
Since causes of maternal deaths are not always investigated, it is difficult to know exactly how many occur each year. However, medical professionals estimate their occurrence to be between one and 12 in every 100,000 deliveries. We still don’t know all of the reasons that they occur, but research has identified a few potential risk factors, including:
- Increased maternal age – Research suggests that mothers over the age of 35 may be at a greater risk of experiencing an amniotic embolism. Maternal age at birth has been increasing over the last decade, which could explain why the increasing prevalence of amniotic embolisms.
- Preeclampsia – High blood pressure and excess protein in the urine may increase a mother’s risk of experiencing an amniotic embolism, but doctors are uncertain as to why the link exists.
- Placenta problems – Abnormalities in the uterus or placenta (i.e. placenta previa, placenta abruption, etc.) disrupt the barrier between you and your baby, which could ultimately increase your risk of developing an amniotic embolism during childbirth.
- Medically induced labor – While research on the potential link between medically induced labor and amniotic embolisms are conflicting, there is some evidence to suggest that it could increase your overall risk. As such, it may be best to avoid induction (if possible) if you have other factors that increase your chances of experiencing an amniotic embolism.
- Polyhydramnios – This condition causes too much amniotic fluid around your baby, and it could increase your risk of developing an amniotic embolism during childbirth.
- Extensive delivery measures – Operative measures like cesarean sections and vacuum extractions disrupt the barrier between you and your baby. They may also increase your overall risk of developing an amniotic embolism. As such, you may want to avoid such measures (if possible) when other risk factors are present.
Sadly, there is no test to determine your risk for an amniotic embolism, nor is there one to detect whether one has occurred during your birth. Instead, the presence of the condition typically goes undetected until it is too late, which is why the mortality rate is so high.
“It is an unforeseeable complication of pregnancy, and the only thing you can do if the mother collapses is to do the kinds of life support that you would do with an intensive care unit, trying to hope that that will get her through the crisis,” Dr. Jennifer Blake, chief executive of the Society of Obstetricians and Gynecologists, told CBC News shortly after Jenkins’ death. “We really don’t have any specific cure or remedy. It’s really trying to keep the heart pumping and the blood circulated.”
And even mothers who manage to survive an amniotic embolism are at risk for serious complications, including severe and permanent brain trauma, extended hospital stays, and even death of the baby.
Minimizing Your Risks – Is It Possible?
With no way to really detect the presence or potential risk of an amniotic embolism, mothers must rely on the signs and symptoms to reduce their risk. If you or your support system notice any of these symptoms during or immediately after your birth, notify a nurse immediately:
- Sudden drop in blood pressure,
- Sudden shortness of breath,
- Chills,
- Altered mental state (anxiety, a sense of doom, etc.),
- Rapid heart rate,
- Disturbances in the rhythm of heart rate,
- Seizure,
- Loss of consciousness,
- Bleeding from the uterus,
- Bleeding from an IV site,
- Bleeding from a cesarean incision,
- Blood clotting,
- Fetal distress,
- Failure of the heart to effectively pump blood.
The Bottom Line
While we may not be able to outright prevent or detect amniotic embolism, increased awareness and more investigations into the unexplained deaths of healthy mothers could bring us to a place where amniotic embolisms are a thing of the past. Until that time, be aware and talk to your doctor about your potential risk factors and the possibility of a monitoring plan.