 Sometimes a preemie doesn’t need to be hooked up to 10 different machines to be given the chance to survive.
Sometimes a preemie doesn’t need to be hooked up to 10 different machines to be given the chance to survive.
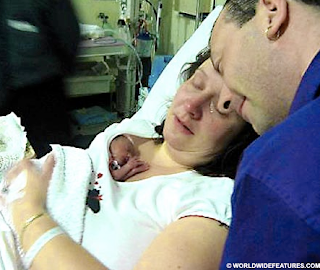
When Carolyn Isbister put her 20oz baby on her chest for a cuddle, she thought that it would be the only chance she would ever have to hold her. Doctors had told the parents that baby Rachel only had only minutes to live because her heart was beating once every ten seconds and she was not breathing.
Mrs. Isbister remembers saying:
“I didn’t want her to die being cold. So I lifted her out of her blanket and put her against my skin to warm her up. Her feet were so cold.
“It was the only cuddle I was going to have with her, so I wanted to remember the moment.” Then something remarkable happened. The warmth of her mother’s skin kick started Rachael’s heart into beating properly, which allowed her to take little breaths of her own.
“We couldn’t believe it – and neither could the doctors. She let out a tiny cry.”
“The doctors came in and said there was still no hope – but I wasn’t letting go of her. We had her blessed by the hospital chaplain, and waited for her to slip away.
“But she still hung on. And then amazingly the pink colour began to return to her cheeks.”
“She literally was turning from grey to pink before our eyes, and she began to warm up too.”
The sad part is that when the baby was born, doctors took one look at her and said ‘no’.
“They didn’t even try to help her with her breathing as they said it would just prolong her dying. Everyone just gave up on her,” her mom remembered. Ian Laing, a consultant neonatologist at the hospital, said: “All the signs were that the little one was not going to make it and we took the decision to let mum have a cuddle as it was all we could do.
“Two hours later the wee thing was crying. This is indeed a miracle baby and I have seen nothing like it in my 27 years of practice. I have not the slightest doubt that mother’s love saved her daughter.”
Rachael was moved on to a ventilator where she continued to make steady progress.
Miss Isbister said: “The doctors said that she had proved she was a fighter and that she now deserved some intensive care as there was some hope.
“She had done it all on her own – without any medical intervention or drugs.
“She had clung on to life – and it was all because of that cuddle. It had warmed up her body enough for her to start fighting.”
Because Rachel had suffered from a lack of oxygen doctors said there was a high risk of damage to her brain. But a scan showed no evidence of any problems.
After just 5 weeks she was taken off the ventilator and four months she was released home.
She is currently doing well and enjoys cuddles, which her parents give whenever possible.
When a parent holds their baby on their chest – skin to skin it is referred to as Kangaroo Mother Care.
The benefits for all babies on KMC are that they stabilize faster on skin to skin care than in the incubator (they do not stabilize in the incubator in the first six hours of life)Then KMC babies have stable oxygen rates and breathing. The heart rate is stable. The temperature is most stable on the mother ( in skin to skin care the mothers chest automatically warms to warm a cold baby, and the mothers core temperature can drop if her baby has a temperature.)
You can read more about it at kangaroomothercare.com







I am so glad that your baby Rachel is doing well!!
As a nurse in a large NICU, we know from statistics that most 23 wk gest. neonates do not survive, and most have severe disabilities. But some can and do survive, and thrive.
It is important to find out, and visit the hospital you will be using, does it have a NICU, what are their policies.
Some hospitals do not resuscitate below say 26 weeks. I know in my hospital that if the baby is perceived viable, and the parents ask for everything done, we try our hardest. We will, and do care for 23 weekers. I do not know what hospital this was, and i am sorry to hear that they would treat a mother this way.
We encourage kangaroo care, and breastmilk/breastfeeding. and we are looking into providing banked breast milk for the micropreemies whose mother’s are unable to produce milk (either for physical or medical reasons).
We also participate in groups throughout the world (Vermont Oxford, and Ideal NICU) that study what NICU’s are doing to make vast improvements (in survival, in treatments, in infections etc…). We are a group of hospitals with very good success statistics, and we study share this info, so that other NICU’s can share the same successes.
I hope that you all understand, we in the medical community want all these babies to survive and thrive and do well, we LOVE to see them grow, we love updates, and pictures, and visits… to see these “miracles” grow bigger and stronger.
I love this story. I had a similiar experience with my sixth child. I had to fight for the chance to hold her b/c she was a premie and sickly. Her temp was not going up and I knew as a mother that my baby needed my touch.
I fought to hold her and NICU finally allowed me the opportunity. She immediately began to transform.
Here we can see what love and the kangooro care can make. All machines we have in the rich world is not always the best thing. Love is the greatest.
I just wrote about this in my blogg 2 days ago (in swedish, unfortunately) and I have read about this type of caring before.
It’s a miracle!
Kao (from Sweden)